- Author Jason Gerald gerald@how-what-advice.com.
- Public 2024-01-19 22:11.
- Last modified 2025-01-23 12:04.
Many women experience bleeding at some point in their pregnancy, especially in the first trimester. In most cases (especially in the early stages, and if the bleeding is not too severe), this is considered normal. However, continued bleeding can be alarming and should be seen by a doctor, especially if the bleeding is accompanied by pain, cramping, fever, dizziness, or fainting. You should know the strategies needed to manage and control bleeding if it occurs, in addition to contacting your doctor at the right time for additional help and treatment.
Step
Method 1 of 2: Analyzing and Controlling Bleeding
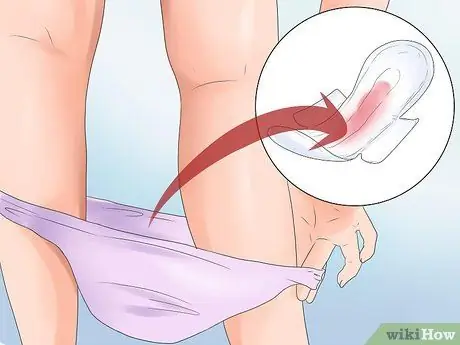
Step 1. Watch the progress of bleeding
You must know the amount of blood that comes out when bleeding occurs. In this way, the doctor will be able to diagnose and determine the appropriate follow-up plan. Begin to pay attention to the amount of blood that comes out, as soon as bleeding occurs.
- You can do this by tucking medical pads in your underwear. Count the number of wet pads from 8 a.m. to the same time the next day. Record the results, then take them to the doctor for examination purposes.
- Also take note of other characteristics of the bleeding, such as whether you feel pain or not, and whether the bleeding is constant or intermittent. This information will be useful for the doctor to determine the cause of the bleeding.
- Pay attention to the color of the blood (pink versus red versus brown), as well as the presence/absence of clots or other "body tissue" that may have come out with the blood. If there is body tissue that comes out of the vagina along with blood, you can collect it in a container to show the doctor, as this can help him diagnose the cause of the problem.

Step 2. Take frequent breaks
Rest is the ideal treatment period for bleeding in the early days of pregnancy. Doctors usually recommend full rest for the first few days after bleeding starts.
If the bleeding doesn't stop or goes away after resting, you should see a doctor for a more detailed analysis
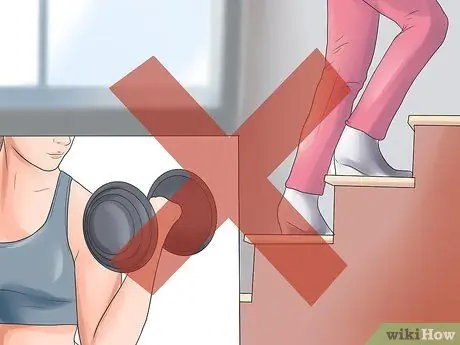
Step 3. Avoid heavy work
The doctor will advise you to avoid heavy work such as lifting weights, climbing stairs regularly, running, cycling, etc. These activities cause sudden movements of the uterus and can tear the newly formed blood vessels in the placenta. Avoid these measures, even if your bleeding is light.
You should still limit physical activity and avoid strenuous work for at least two weeks after the bleeding occurs

Step 4. Don't have sex for a while
Sexual intercourse can sometimes spur or worsen bleeding.
If you experience bleeding during pregnancy, avoid sexual intercourse until your doctor thinks it can be done. Usually, you should wait at least two to four weeks after the bleeding stops

Step 5. Do not use tampons or other inserts
Do not insert anything into the vagina after bleeding has occurred. Avoid tampons at all times, because tampons can injure the walls of your vagina or uterus, making your bleeding worse. The inserted object can also carry bacteria and other microorganisms into the vagina, so you have a serious infection.

Step 6. Stay hydrated
You should drink adequate amounts of fluids when you are bleeding, especially if the bleeding is very severe.
- Drink at least eight cups of water every day to stay hydrated. Bleeding is related to fluid loss, so you'll need to drink more than usual to replace fluids that come out.
- You also need to stay hydrated for your baby to be healthy.
Step 7. Be aware of the causes of bleeding during pregnancy
This way, you can tell what happened in your case.
- Bleeding is quite common in the first trimester (12 weeks after pregnancy) and affects 20-30% of women. Most of these cases are harmless, meaning there is no risk to the mother or the baby, and may occur due to the attachment of the fetus to the uterine wall/other physiological changes during pregnancy.
- However, there are some more worrying possibilities associated with heavy bleeding and/or pain in the first trimester. Some examples are "ectopic pregnancy" (a baby implanted with a fallopian tube instead of a uterus), "molar pregnancy" (a rare condition that causes abnormal tissue - not a fetus - to grow in the uterus), or miscarriage.
- 50% of bleeding in the first 20 weeks of pregnancy indicates miscarriage.
- Bleeding later in pregnancy (in the second or third trimester) is more worrying. Some of the causes include problems with the placenta, uterus (especially if you've had a C-section), premature birth (before 37 weeks), or due to a normal delivery (if you're close to your due date).
- Other causes of bleeding may not be related to pregnancy, eg "trauma" (or injury to the vaginal wall) as a result of sexual intercourse, cervical polyps (flesh growths that may bleed and may or may not appear in pregnant women), cervical dysplasia (abnormal cells that can lead to cancer), and/or cervical cancer (which is one of the most common types of cancer in women that is not routinely screened for with a Pap test).
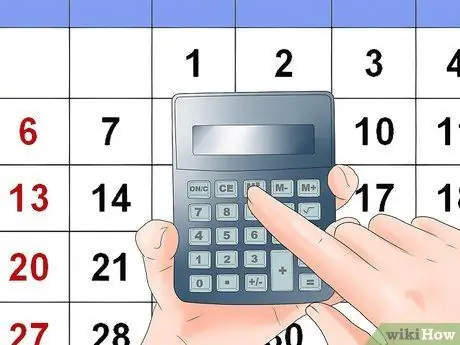

Step 8. Calculate your estimated due date and consider whether bleeding means you are ready to give birth
Pregnancy usually lasts for 40 weeks or 280 days. You can use this information to calculate your approximate due date - just add 9 months and 7 days from the first day of your last period. For example, if your last period started on January 1, 2014, your estimated due date would be October 8, 2014.
Bleeding around your due date may indicate that you are ready to give birth. The range is generally from 10 days before to 10 days after the estimated date. You should report to your doctor immediately if you think you are ready to give birth

Step 9. Know when to ask a medical professional for help
All bleeding during pregnancy should be discussed with the doctor within a normal time frame. If the bleeding is accompanied by any of the following symptoms, you should immediately see a doctor in the ER for examination and treatment:
- Severe pain or cramping
- Dizziness or fainting (signs of massive bleeding)
- Tissue that comes out of the vagina along with blood (may indicate a uterine error)
- Fever and/or chills (may indicate infection)
- Severe bleeding that doesn't stop or slows down.
Method 2 of 2: Knowing the Right Time to Ask for Medical Help

Step 1. Know that you can ignore very light bleeding
If your bleeding is light (just a few drops), it's usually brown and lasts less than a day or two, and there's no pain or cramping, so you can ignore it. Usually this bleeding is caused by implantation or dilated blood vessels.
Regardless of how small the bleeding is, you should avoid strenuous work for a few days and monitor the amount of blood that comes out

Step 2. Get medical help if you have heavy bleeding
Any type of heavy bleeding during pregnancy should be considered an emergency. Heavy bleeding is defined as bleeding that is more than bleeding during menstruation.

Step 3. Watch for any pain or cramping that may arise
Pain that comes and goes indicates uterine contractions, which means your uterus is trying to expel the fetus. In the early days of pregnancy, pain and cramping can be a sign of uterine abnormalities. In the third trimester, these signs may indicate that you are ready to give birth. So, if you experience pain or cramping, call your doctor right away.
The pain of childbirth will occur regularly at certain intervals. This pain will increase in intensity and duration gradually and is associated with mucus mixed with blood

Step 4. Seek help if you are dizzy or faint
Feeling dizzy or fainting is a symptom of a large amount of blood loss.

Step 5. Check body temperature
Bleeding accompanied by fever usually indicates infection, for example in the uterus due to an abnormal pregnancy or abortion. Therefore, all cases of fever should be notified to the doctor immediately.

Step 6. Seek immediate help if you are expelling body tissue through the vagina
This is an indication of a serious content error. If this occurs, call your doctor so he or she can evacuate the uterus if necessary, so that your bleeding is under control.

Step 7. Follow the doctor's post-treatment instructions
Regardless of the cause of the bleeding (whether due to an uterine error, an ectopic pregnancy outside the uterus, an infection, or close to delivery), your body will be under stress. In general, the doctor will recommend rest, forbid strenuous exercise/sexual intercourse, and tell you to drink lots of water. Make sure you listen to your doctor's advice so you can maximize the speed of your body's recovery, as well as prevent further complications.






