- Author Jason Gerald gerald@how-what-advice.com.
- Public 2024-01-19 22:11.
- Last modified 2025-01-23 12:04.
Mastitis is an inflammation of the breast tissue that causes the breast to feel sore and swollen. Mastitis generally occurs in nursing mothers, when bacteria enter the breast through an injured nipple or as a result of milk remaining in the breast after breastfeeding. Mastitis can be prevented through good breast and nipple care and by ensuring that the breasts are completely empty after feeding.
Step
Method 1 of 3: Proper Breastfeeding to Prevent Mastitis

Step 1. Learn how to breastfeed properly from a healthcare professional
Mastitis can occur at any stage of the breastfeeding process, but many women experience it in the first four weeks of breastfeeding, when their breasts enlarge. This often happens to mothers who gave birth to their first child, so that they are breastfeeding for the first time. Talk to your doctor or midwife to find out how to breastfeed properly so you can prevent mastitis.
- Early in your pregnancy, your doctor or midwife will likely provide you with manuals and information that will prepare you during pregnancy, labor and the first weeks after delivery. If they don't provide you with this guide, then ask for it.
- After your baby is born, don't hesitate to talk to a healthcare professional if you need to learn to breastfeed. You can also use the internet to find useful information. There are many websites specifically designed to provide pregnancy and breastfeeding information. Many of them offer a sign-up program, where if you sign up, you'll receive weekly emails as you progress through your pregnancy.

Step 2. Feed your baby according to a regular schedule to avoid getting your breasts overfilled with milk
Full breasts can cause them to enlarge and trigger mastitis. You should breastfeed your baby every one to three hours, or whenever your baby is hungry.
If you know that you will miss a feeding session, be sure to pump your milk to empty the breasts

Step 3. Encourage your baby to feed whenever you feel your breasts are full
If your breasts are full before your usual feeding schedule, then you need to empty them. If milk is stored in the breast, it will thicken, blocking its flow and possibly triggering mastitis.
- You don't have to wait for your baby to give you signs of hunger. Your baby will likely not refuse milk when offered the breast, even if it's not the time to feed.
- Don't be afraid to wake your baby up if you need to. It is better to disturb your baby's sleep and empty the breast than to run the risk of mastitis which will cause pain.

Step 4. Let your baby suckle as long as it takes to empty your breast
All babies have different feeding needs and all mothers have different milk flows. Some babies can empty their milk in as little as 10 minutes, while others can suckle for 30 minutes on each breast. Recognize your baby's feeding needs and allow him or her to spend the necessary time emptying your breasts.
Don't watch the clock or set a time limit for breastfeeding just to keep your feeding schedule. Take the time it takes your baby to completely empty your breast

Step 5. Begin the breastfeeding session by offering a different breast
If you offered the left breast the last time you breastfed, offer the right breast the next feeding session. Changing breasts will reduce your chances of developing mastitis.
Sometimes you may be confused about which breast you were last offered to your baby. Some mothers find it easier to remember by wearing the "nursing bracelet" on the wrist of the first offered side. Nursing bracelets are available for sale at maternity boutiques, but you can use any bracelet if you don't have one
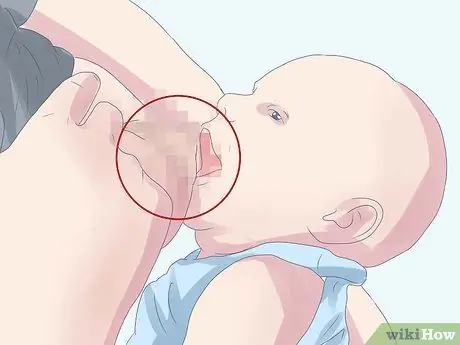
Step 6. Make sure that your baby is latched on to the breast properly
An imperfect latch can affect the nipple and interfere with the flow of milk. Look in various sources for information on the correct attachment technique. If your baby is having trouble latching on well, consult a lactation consultant.
- To latch on properly, your baby must be positioned up, with his chest pressed against yours.
- If your areola is not protruding, massage your breast to make it protrude so your baby can latch on well.

Step 7. Help your milk flow by massaging your breasts
Gently massage your breast before latching on to help the let down reflex and help the milk flow smoothly.

Step 8. Change your position during the feeding session
Try different feeding positions and use a pillow during feedings so you can breastfeed comfortably and easily. It also helps to ensure that your breasts will empty completely at each feeding session.

Step 9. Avoid bottle feeding your baby during the time between feedings
You need to empty your breasts as much as possible, and the baby is the winner.
- If you use a bottle between feedings, your baby will be less hungry to empty your breast. This can put you at risk for breast enlargement.
- In addition, offering a bottle of milk can cause nipple confusion as your baby will try to use both nipples when feeding.
- What's worse, your baby may prefer to feed from a bottle, because the flow of milk from the bottle is smoother, so the baby becomes lazy to suck. The baby may even refuse the breast or have difficulty sucking the breast.
Method 2 of 3: Keeping Your Body Healthy

Step 1. Sleep comfortably
Try not to sleep in a position that puts pressure on your breasts, and avoid sleeping in a bra. This can put pressure on the sensitive mammary glands, causing them to become inflamed. If inflammation occurs, the milk ducts can become blocked, which then leads to mastitis.
- The best position for sleeping is on your back, but if you like to sleep on your side, use a bolster to help you get into a comfortable sleeping position without pressing your breasts.
- When you feel your breasts full at night, get up and feed your baby.
Step 2. Take time to release stress
As a new mother, you will likely be overwhelmed with caring for your baby. While you need to make sure that your baby's needs are met, you likely can't do the same for yourself. So making time to take care of yourself is also important. Because if your immune system is compromised, you will be more at risk of suffering from mastitis.
- Increase your sleep time, drink plenty of fluids and eat healthy foods. Take your pregnancy vitamins while breastfeeding.
- If you feel overwhelmed, take a 10-minute break from your baby so you can control yourself and breathe easy.

Step 3. Avoid tight tops or bras that put too much pressure on your body
Do not wear a bra as often as you can to avoid putting pressure on the milk ducts. Wear loose, comfortable clothing so you don't press against your breasts.
Step 4. Treat sores on the nipples
Nipples are often injured during breastfeeding, and these open sores can be an entry point for bacteria and cause mastitis. Prevent and treat sores on the nipples by doing the following:
- Allow your breasts to air dry after feeding. This will be better than wiping it with a towel or washing it every time you feed it, which can cause it to dry out too much.
- Wipe with lanolin cream. Look for natural, alcohol-free creams to treat sore and dry nipples.
Method 3 of 3: Recognizing the Signs of Mastitis

Step 1. Check for inflammation, redness or swelling
These symptoms often occur when the milk ducts become blocked before the onset of mastitis. Detecting these symptoms as early as possible can really help you to take steps to treat this problem before mastitis occurs.

Step 2. Pay attention to any pain you may feel
Determine if this occurs in a specific area or throughout your breast. If you find that this is only happening in certain areas, then it may be due to a blocked milk duct.
- Apply a warm compress to the sore area daily, and make sure to completely empty your breast with each feeding.
- If your breast inflammation does not subside, see a doctor immediately.

Step 3. Notice if your breasts feel hard or hot to the touch
Even without pain, hard, tender breasts are an early sign of an infection.

Step 4. Pay attention if you feel unwell
Sometimes mastitis can appear suddenly. Headache, chills, body aches, and fatigue are possible markers of mastitis.

Step 5. Take your temperature if you feel sick or unwell
A body temperature of more than 38 degrees Celsius can be a sign that a mastitis infection is occurring.

Step 6. See a doctor if your symptoms do not subside
If your breasts are getting worse, your fever is rising, or you feel sicker over time, you may have a mastitis infection and should seek medical attention.
- You need to continue breastfeeding, even if you have an infection. Stopping breastfeeding can make the problem worse. Talk to your doctor for ways to reduce pain.
- If your doctor states that your mastitis is caused by an infection, he or she may prescribe antibiotics.






