- Author Jason Gerald gerald@how-what-advice.com.
- Public 2023-12-16 10:50.
- Last modified 2025-06-01 06:05.
Crohn's disease, a type of inflammatory bowel disease, is a condition in which the lining of your digestive system becomes inflamed, causing severe diarrhea and abdominal pain. The inflammation sometimes spreads into the layers of the affected tissue. Like ulcerative colitis, another inflammatory bowel disease, Crohn's disease can be painful and debilitating and can sometimes lead to life-threatening complications.
Although no cure has been found for Crohn's disease, medication can reduce the signs and symptoms of Crohn's disease and may even provide long-term relief. With this treatment, many people with Crohn's disease can carry out normal activities of daily living.
Step
Part 1 of 2: Recognizing the Symptoms and Confirming the Diagnosis
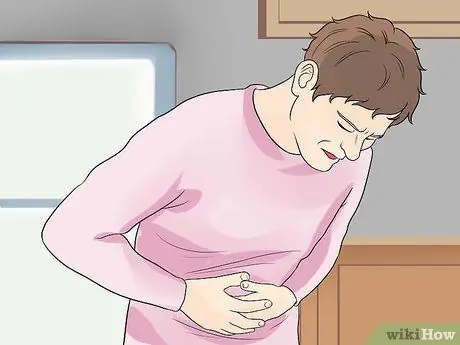
Step 1. Know the signs and symptoms of Crohn's disease
Symptoms of Crohn's disease are similar to those of other bowel diseases, such as ulcerative colitis and irritable bowel syndrome. Symptoms can come and go and vary from mild to severe. Symptoms will be different for each person, depending on which part of the intestinal system is infected. Some of the common symptoms include:
-
Diarrhea:
The inflammation that occurs in Crohn's disease causes cells in the affected areas of your intestines to excrete large amounts of water and salt. Since the large intestine cannot absorb excess fluid completely, this results in diarrhea.
-
Abdominal pain and cramps:
Inflammation and ulcers can cause the walls of some parts of your intestines to swell and eventually become thick with scar tissue. It affects the normal movement of the intestinal system through your digestive system and can cause abdominal pain and cramps.
-
Blood in the bowel:
Food passing through your digestive system can cause inflamed tissue to bleed, or your intestines may bleed on their own.
- Ulcer (ulcer) Crohn's disease starts as small, spreading sores on the surface of the intestine. Later this wound becomes an ulcer that goes into --- and sometimes penetrates --- the intestinal wall.
-
Decreased appetite and weight:
Abdominal pain and cramping and the inflammatory reaction of your intestinal wall can affect your appetite as well as your ability to digest and absorb food.
-
Fistula or abscess:
Inflammation from Crohn's disease can pass through the intestinal wall into adjacent organs, such as the bladder or vagina, causing an abnormal connection called a fistula. This mass also causes abscesses; sores that are swollen and festering.

Step 2. Recognize the less common symptoms of Crohn's disease
In addition to those mentioned above, people with Crohn's disease may experience other, less common, symptoms such as joint pain, constipation, and swollen gums.
- People with severe Crohn's disease may experience fever and fatigue, as well as problems that occur outside the digestive system, including arthritis, eye inflammation, skin disease, and inflammation of the liver or bile ducts.
- Young children with Crohn's disease may have stunted growth or sexual development.

Step 3. Know when to seek medical advice
Call your doctor right away if you experience any of these symptoms:
- Feeling weak and having a fast or slow pulse.
- Severe stomach pain.
- Unexplained fever or chills that last more than a day or two.
- Repeated vomiting.
- Blood in the toilet.
- Chronic diarrhea that doesn't stop with over-the-counter medications.

Step 4. Perform tests to confirm the diagnosis
If your doctor suspects you may have Crohn's disease, he or she may refer you to a gastroenterologist (a specialist in the digestive system) for different diagnostic tests. This may include:
-
Blood test:
Your doctor may recommend blood tests to check for anemia, which is a common side effect of Crohn's disease (due to heavy blood loss).
-
Colonoscopy:
This exam allows your doctor to view your entire colon using a thin, flexible tube attached to a camera. With the camera, the doctor will be able to identify inflammation, bleeding or ulcers in the colon wall.
-
Flexible sigmoidoscopy:
In this procedure, your doctor uses a thin, flexible tube with a light to observe the sigmoid, which is the last 2 legs of your large intestine.
-
Barium enema:
This diagnostic test allows your doctor to evaluate your colon with an X-ray. Before the test, barium, a contrast dye, is inserted into the intestine with an enema (injection).
-
Small intestine X-ray:
This test uses an X-ray to examine the part of the small intestine that is not visible from a colonoscopy.
-
Computerized Tomography-Computational Tomography (CT):
Sometimes you will need a CT scan, which is a special x-ray technique that provides more detail than a standard x-ray. This examination shows the entire intestine as well as tissue outside the intestine that cannot be seen with other tests.
-
Capsule endoscope:
If you have signs and symptoms similar to Crohn's disease, but the general diagnostic test is negative, your doctor may perform a capsule endoscopy.
Part 2 of 2: Understanding Treatment Options

Step 1. Ask your doctor about drug therapy
Many different medications are used to control the symptoms of Crohn's disease. The type of medication that is right for you will depend on the state of Crohn's disease and the severity of your symptoms. Some of the commonly used treatment drugs are as follows:
-
Anti-inflammatory drugs:
This drug is commonly used as the first step in treating inflammatory bowel disease. It contains sulfasalazine (Azulfidine) which is especially useful for bowel disease, mesalamine (Asacol, Rowasa) which can help prevent recurrence of Crohn's disease after surgery, and corticosteroids.
-
Immune system defense:
This drug also reduces inflammation, but it targets your immune system first rather than treating the inflammation itself. It contains azathioprine (Imuran) and mercaptopurine (Purinethol), infliximab (Remicade), adalimumab (Humira), sertolizumab pegol (Cimzia), methotrexate (Rheumatrex), cyclosporine (Neoral, Sandimmune), and natalizumab (Tysabri).
-
Antibiotics:
It can cure fistulas and abscesses in people with Crohn's disease. It contains metronidazole (Flagyl) and ciprofloxacin (Cipro).
-
Anti-diarrhea medicine:
Crohn's disease patients who have chronic diarrhea usually respond well to anti-diarrheal agents such as loperamide. Loperamide - which is traded as Imodium - can be purchased over-the-counter without a prescription.
-
Bile acid separator:
Patients with late ileal disease or with previous resection of the ileum (the end of the small intestine) may not absorb bile acids normally which can lead to diarrhea with intestinal discharge. These patients may be assisted by bile acid separators such as cholestyramine or colestipol.
-
Other Medications:
Some other medications that can relieve the symptoms of Crohn's disease include steroids, immune system boosters, fiber supplements, laxatives, pain relievers, iron supplements, vitamin B12 injections, and calcium and vitamin D supplements.

Step 2. Follow your doctor's advice regarding diet and nutrition
There is no solid evidence that what you eat actually causes inflammatory bowel disease. But certain foods and drinks can make the disease worse (especially when it's overdone) but others can relieve symptoms and prevent future flare-ups.
- Fiber supplements are said to be beneficial for patients with bowel disease. This is because fiber can be converted into short fatty acids, which help the intestines heal itself.
- Try to avoid dairy products, as most patients with Crohn's disease (especially of the small intestine) cannot digest lactose. You can take calcium supplements to treat deficiencies and reduce your risk of osteoporosis.
- Avoid foods that usually cause gas and bloating such as beans and green leafy vegetables. You should also limit fatty, oily, or fried foods that can interfere with healthy digestion. In addition, you should also try to eat smaller portions, to minimize bloating and avoid straining your digestive system.
- In certain situations, your doctor may recommend a special diet that is given through a feeding tube (enteral) or nutrition by injection (parenterally) to treat your Crohn's disease. This is a temporary nutritional supplement, usually for people whose intestines have to rest due to surgery, or whose intestines fail to absorb nutrients on their own.
- Be aware that each Crohn's disease patient is different and may have their own unique food intolerances. A good way to identify the intolerance is to have a daily food journal in which you record everything you eat. This helps you identify foods that make your symptoms worse. Once you know which foods are causing your symptoms, you can try to avoid them.
Step 3. Make some lifestyle changes
Although there is no cure for Crohn's disease, you can minimize your symptoms and live a long, normal life by following your doctor's treatment advice and making healthy lifestyle choices. This includes:
-
Reduce stress:
While stress doesn't cause Crohn's disease, it can worsen your signs and symptoms and can cause flare-ups. While it's not always possible to avoid stress, you can learn how to deal with it.
-
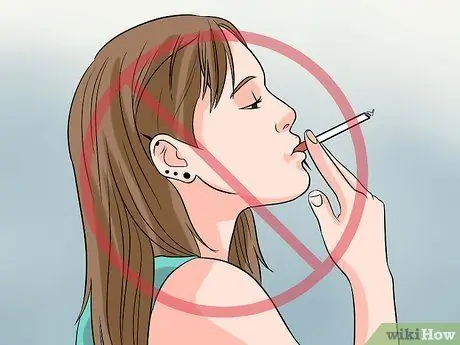
Quit smoking:
If you smoke, you are more at risk of developing Crohn's disease. In addition, smoking worsens the symptoms of Crohn's disease, and increases the risk of complications and surgical intervention.
-
More sports:
Regular exercise will help you maintain a healthy weight and reduce stress - two things that can make a big difference in controlling disease. Try to find a form of exercise that you enjoy - whether it's a dance class, rock climbing, or dragon boat racing.
-
Avoid drinking alcohol:
Symptoms of Crohn's disease can worsen as a result of drinking alcohol. Therefore, it is recommended that you only drink in moderation, or not drink at all.

Step 4. Research surgical treatment
If dietary and lifestyle changes, drug therapy or other treatments don't relieve your signs and symptoms, your doctor may suggest surgery to remove the damaged part of your digestive system to close the fistula or remove scar tissue. There are three main types of surgery that Crohn's patients undergo:
-
Proctoecectomy:
This procedure involves removing part of the rectum and all or part of the intestine. This is done with the patient under general anesthesia by a specialist surgeon. Recovery time is usually between 4-6 weeks.
-
Ileostomy:
An ileostomy is the second procedure performed after a proctoecectomy. This involves attaching the ileum (the end of the small intestine) to the opening of the abdomen (called a stoma). A small pouch (called a stoma sac) is attached to the stoma to collect feces. After surgery, the patient will be shown how to empty and clean the bag, and can continue to live a healthy and normal life.
-
Intestinal resection surgery:
This type of surgery involves removing only the diseased portion of the intestine. Once removed, the two healthy halves are attached, allowing the intestines to resume normal function. Recovery usually takes 3-4 weeks.
- The NIH estimates that approximately 2/3 of people with Crohn's disease will need surgery in their lifetime, when they fail to respond to other treatments. Unfortunately, the disease often recurs after surgery, so further treatment may be required.

Step 5. Try herbs that may be helpful for Crohn's disease:
Herbs like Glycyrrhiza glara, Asparagus racemosus etc. can be beneficial in Crohn's disease.
- Studies on Glycyrrhiza glabra (liquorice) say that this herb can normalize the intestines by reducing inflammation and helping the intestines heal.
- Studies on Asparagus racemosus say that this herb can soothe the gastric mucosal lining and help repair stressed and damaged tissues.
- The study on Valeriana Officinalis says that Advanced Resonance Homeopathic-Homeopathic Resonance Medicine can relieve symptoms such as abdominal pain, constipation, diarrhea, uncontrolled bowel movements, and nausea.
- A study on Veratrum Album says that this Advanced Resonance Homeopathic remedy can relieve loose and watery stools.
Tips
- Increase your knowledge and build relationships with organizations to gain access to support groups.
- Visit your doctor regularly and do blood tests to check for side effects from your medication.
- You are at high risk if you have a close family member, such as a parent, sibling or child, with the disease.
- Regular exercise can help maintain a healthy diet and help relieve stress.
- Alcohol has a strong effect on Crohn's disease. It is recommended, even in everyday life, not to drink to excess or not to drink at all to reduce Crohn's symptoms.
- If you smoke, you are more at risk of developing Crohn's disease.
- Only take medications that are prescribed by a doctor or gastroenterologist.
- Crohn's disease can strike at any age, but you are more likely to develop the condition at a young age.
- Keep a daily food journal containing your food intake to help you remember foods that increase your symptoms and try to avoid them (each Crohn's patient is different).
- Although white people have the highest risk of this disease, it can affect any ethnicity.
- If you live in an urban area or an industrialized country, you are more at risk of developing Crohn's disease.
Warning
- Use anti-diarrhea with extreme caution and only after consulting your doctor, as this increases the risk of toxic megacolon, a life-threatening intestinal inflammation.
- Talk to your doctor before using laxatives, because even over-the-counter ones can be too harsh for your system.
- Do not take anti-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen (Advil, Motrin, etc.) or naproxen sodium (Aleve). This is more likely to make your symptoms worse.






