- Author Jason Gerald gerald@how-what-advice.com.
- Public 2023-12-16 10:50.
- Last modified 2025-06-01 06:05.
The two muscles that work together in the lower leg (or calf) are the inner soleus muscle and the gastrocnemius muscle, which are more visible because they are closer to the skin. These muscles connect the heel to the back of the knee and play a role in plantar flexion of the ankle as well as in knee extension, which is required when we walk, run, jump, and kick. Injuries from a torn calf muscle usually occur in the center of the calf and/or the knee within the muscle "belly". Muscle tears are categorized into grade I (torn muscle), grade II (greater damage to the muscle fiber), or grade III (muscle that has been severed). Getting a definite diagnosis of your torn calf muscle is important, as it will determine the type and steps you should take to treat it.
Step
Part 1 of 4: Consult the Experts

Step 1. Schedule an appointment with your doctor
If you have calf pain for several days, schedule an appointment with your family doctor. The doctor will examine your leg and calf muscles, ask about your lifestyle and assess the process of your injury, and may take an X-ray of your lower leg (to check for fractures of the tibia and fibula). If necessary, the doctor will refer you to a muscle and bone specialist (musculoskeletal specialist), who has special expertise and education in this area.
Other areas of healthcare professionals who can help diagnose and treat muscle injuries include osteopathic therapists, chiropractors, physiotherapists, and massage therapists. However, you should always start this process with your doctor, because the doctor can find other factors that have the potential to cause/indicate a more serious condition, such as blood clots, vascular (blood vessel) injury, cysts (Baker's cyst), or other possible conditions. surgical emergency such as compartment syndrome

Step 2. Talk to an expert about your foot problem
Injury to the calf muscle usually only occurs due to a mild grade I strain, but sometimes requires surgery if the muscle is seriously torn. In fact, serious medical conditions can cause calf pain or other pain in the area, such as fractures, bone cancer, bone infection (osteomyelitis), venous insufficiency, sciatica due to a herniated disc or other complications associated with diabetes. In these cases, medical personnel such as an orthopedic (bone and joint specialist), neurologist (neurologist) or a physiatrist (muscle and bone specialist) are needed to find the most serious cause of your calf pain.
- X-rays, bone scans, MRI, CT scans and ultrasound are tools that medical professionals use to help diagnose pain in your lower limbs.
- Calf muscle injuries are common among tennis, basketball, football, and volleyball players, as well as in runners and other field athletes.

Step 3. Understand the different types of treatments available
Make sure that your doctor gives a clear explanation and diagnosis, especially regarding the cause (if possible), and gives you various treatment options according to your condition. Rest and undergoing treatment at home (such as using ice cubes) may be done for the treatment of minor calf muscle tears.
- Do some independent research on the internet about calf injuries (but only use references from websites that have a clear medical reputation) to better understand the condition and better understand the treatment and the expected results.
- Factors that can predispose a person to a muscle tear (or “pull”) are advanced age, previous muscle injury, lack of flexibility, muscle weakness, and fatigue.
Part 2 of 4: Treating a Grade I Calf Muscle Torn
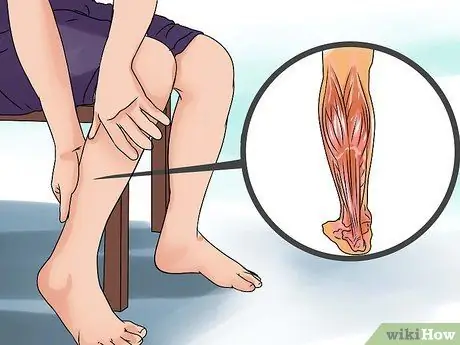
Step 1. Identify how serious your injury is
Most calf muscle tears are minor injuries and will heal on their own within a week - the degree of pain, reduced/loss of muscle function, and bruising are good indicators of how serious it is. Grade I calf muscle tear includes a small tear in the muscle, which is up to 10% of the muscle fiber. Characteristics are mild throbbing pain in the back of the lower leg, usually in the area of the middle leg to near the knee. Patients will experience a slight loss / reduced leg strength and the legs become somewhat difficult to move. You may still be able to walk, run, or exercise, even if it feels uncomfortable and a little stiff.
- A muscle tear occurs when there is force on the muscle that causes the tissue to tear, which usually occurs in the joints between the joints of the muscles that attach to the tendons.
- Most grade I lower leg strains cause discomfort for between two and five days after the injury, but it may take several weeks for recovery to complete, depending on how large the portion of the muscle fiber is affected and the type of treatment.
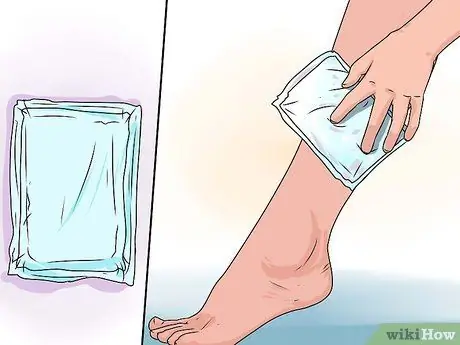
Step 2. Use the “R. I. C. E
"The most effective treatment protocol for most cases of muscle sprains/tears is shortened to R. I. C. E. with the abbreviation "rest (rest)", "ice (ice cubes)", "compression (compress)", and "elevation (lifting)". The first step is rest - stop all activity for a while so that your injury can be treated. Then, treatment is done with cold therapy (using ice cubes wrapped in a thin towel or frozen gel bag as a compress method) on the injury as soon as possible to stop internal bleeding and reduce swelling, and even better if your foot is raised on a bench or pile pillow (so it also helps with swelling). Apply ice for 10-15 minutes every hour, then reduce the frequency within a few days after the pain and swelling subsides. Ice your injury with a compress pad or other elastic material that also helps stop bleeding from torn muscle fibers and reduces swelling.
Do not tie the compress pad too tightly, and only put the compress on for more than 15 minutes at a time, as severely restricted blood flow can cause more serious damage to your leg

Step 3. Buy over-the-counter drugs available in stores
Your doctor may recommend an anti-swelling medication such as ibuprofen, naproxen, or aspirin, or perhaps a common pain reliever such as acetaminophen that helps with swelling and pain from a calf injury.
Keep in mind that these medications are generally not good for your stomach, liver and kidneys, so don't take them for more than two weeks at a time, or take them as directed by your doctor

Step 4. Perform calf stretching exercises
Light muscle tears will respond well to light stretches too, because this kind of exercise relieves muscle tears and helps improve blood circulation. After the swelling phase of the tearing muscle injury, new tissue is formed to replace the injured, but this new tissue is not as flexible as the original muscle fiber. Stretching aids in wound tissue renewal and makes it more flexible. So, take a towel or compress pad and wrap it under your feet near the toes. Then, grab each end with your hands and slowly pull them back while extending your legs. Pay attention to the stretch that occurs on the inside of your calf muscles, hold this position for 20-30 seconds and then slowly relax again. Do this stretching exercise three to five times a day for one week, as long as your calf pain doesn't get worse because of it.

Step 5. Consult your doctor or physiotherapist before doing these exercises and be careful, as these exercises can sometimes make things worse and slow down your healing and recovery process
Warm up and then stretch your calf muscles before doing sports, so you can avoid muscle tearing, sprains and muscle cramps
Part 3 of 4: Treating a Grade II Calf Muscle Torn
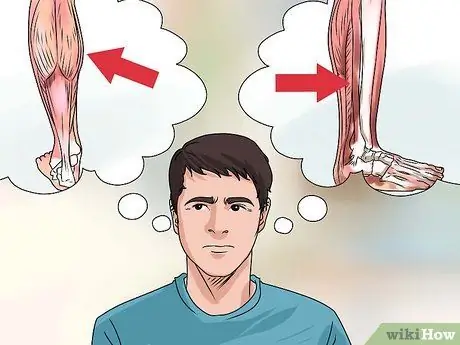
Step 1. Distinguish between gastrocnemius and soleus muscle tears
In more serious muscle tears, it is important to know which muscle is causing the more serious pain: the deep soleus muscle or the superficial “head” of the gastrocnemius muscle. An MRI or ultrasound needs to be done in order to get the best diagnosis in determining the location and extent of the injury. Grade II muscle tears involve more serious damage, with up to a 90% chance of tearing the muscle fibers. This injury causes more serious pain (usually this pain is referred to as “sharper”), and a serious loss of muscle strength and range of motion. There is accelerated swelling and more severe bruising due to internal bleeding from torn muscle fibers.
- In this grade II muscle tear, there is a limitation in the ability to move, especially jumping and running, so you should rest for a while (for a few weeks or more).
- In the case of muscle tears, the gastrocnemius muscle is a high-risk muscle because it lies across two joints (knee and ankle) and has a high proportion of type 2 muscle fiber spasm speed.
- The base of the center of the gastrocnemius muscle is more often strained than the base of the side.

Step 2. Use the “R. I. C. E
This protocol is still appropriate for grade II muscle tears, although you may need to hold the ice cube in the calf longer (up to 20 minutes at a time) if the deep soleus muscle is the primary site of injury. Instead of using the R. I. C. E. for several days as in the case of a mild muscle tear, in the case of a more severe muscle tear it will require a week or more of more attention and duration.
- Most cases of Grade II lower leg muscle tear cause significant discomfort for one to two weeks after the injury, depending on the size of the muscle fiber area and the type of treatment. These types of muscle injuries require one to two months of recovery time so the sufferer can be able to carry out sports activities again.
- In cases of moderate to severe muscle tear, limit the use of anti-inflammatory drugs for the initial 24-72 hours, so as not to increase the risk of bleeding from the effects of anti-platelet drugs (blood thinning drugs).

Step 3. Do physiotherapy
Grade II muscle tears include moderately serious musculoskeletal injuries involving the formation of serious tissue injuries and markedly reduced range of motion and strength. So, once swelling, bruising, and pain have subsided, ask your doctor to refer a sports medicine specialist or physiotherapist who can provide training, stretching, massage techniques, and other therapies such as ultrasound therapy (to reduce swelling and treat tissue injuries) and electronic stimulation of muscles (to strengthen muscle tissue and increase blood circulation), which aims to restore strength to your injured muscles.
- Returning to full activity is usually allowed when you are no longer in pain, your lower leg has full range of motion again, and your calf muscles are strong again. This recovery can take several weeks or more.
- A calf muscle tear usually occurs in men between the ages of 30 and 50.
Part 4 of 4: Treating a Grade III Calf Muscle Torn

Step 1. Seek immediate medical attention
Grade III muscle tear means that the “body” of the muscle or major muscle has been severed. This will cause extreme pain (such as a sharp burning sensation), immediate swelling, serious bruising, muscle spasms, and sometimes a "crackling" sound when the muscle is injured. There is also a palpable flatulence on the calf due to strong contractions of the area experiencing severe pain. The inability to walk is a characteristic characteristic of grade III calf muscle tears, so the help of others is needed when bringing the patient to the hospital or clinic. Muscle fibers cannot reconnect on their own, even with the formation of new tissue after injury, so emergency treatment is required in this case.
- Sudden tearing of large muscles (such as the large Achilles muscle) is often excruciating and feels like you've been shot by a gun or stabbed with a sharp object in the back.
- Severe calf muscle tearing is very likely to result in bruising, which will focus on your leg and make it blackish and bluish in color.

Step 2. Perform surgery
Grade III (and some grade II) muscle tears may require surgery to restore and reconnect the damaged calf and/or large muscles. Time is an important gamble in cases like this, because the more damaged the muscle is and the more severe the impact, the more difficult it will be to restore muscle elasticity to normal again. Moreover, internal bleeding can cause local necrosis (dead tissue around the injured muscle area) and may (although rarely) even lead to cases of anemia (lack of blood) due to excessive bleeding. Major muscle damage in the "belly" part of the muscle will heal faster because of the large volume of blood flow in that area, whereas muscle damage in the tendon area takes longer to heal because it doesn't receive as much blood flow. Go back to the “R. I. C. E.” protocol. after surgery is complete.
- In cases of total muscle damage, recovery of the calf muscles will take about three months or more after surgery and rehabilitation.
- After surgery, you may need to wear a supportive compression boot (boots that provide compression to help your leg recover from a muscle injury or fracture) and should use a cane for a short period of time before training from physiotherapy.
Step 3. Take time for rehabilitation
As in the case of a grade II muscle tear, physiotherapy is required for the restoration of a grade III muscle tear, especially if surgery is required. Under the supervision of a physiotherapist or physiatrist, isometric, isotonic, and dynamic exercise therapy training, all of which are specifically tailored to your condition, can be performed gradually and successively each time as a form of exercise without any pain at all. This exercise will strengthen the calf muscles and return them to their original shape. It can take between 3-4 months to return to sports activities, although there is a high risk of re-injury in the future.
Biomechanism or poor foot posture is the result of a calf injury, so you need to wear special footwear according to the condition of your foot after rehabilitation, to avoid problems in the future
Tips
- Wear the shoe inside your shoe for a few days, to elevate your heel and shorten the injured calf muscle, as well as relieve tension/pain. But don't forget that if worn for too long, this kind of footwear can cause flexion contractures (muscle shortening) in the large Achilles and ankle muscles, causing them to become permanently stiff.
- After ten days post-injury, the new tissue arising from the injury has the same tensile strength as the adjacent muscles, so progressive rehabilitation can begin under the supervision of your doctor and physical therapist.






