- Author Jason Gerald gerald@how-what-advice.com.
- Public 2023-12-16 10:50.
- Last modified 2025-01-23 12:04.
Herpes simplex virus (HSV) is a common sexually transmitted disease (STD). While doctors can manage symptoms, relieve pain, and reduce your chances of transmitting it, there is no cure for this disease. This virus will stay in a dormant condition and can relapse accompanied by symptoms at any time. Find out if you have herpes by considering high-risk behaviors, recognizing the symptoms, and having an STD screening test.
Step
Part 1 of 3: Recognizing the Symptoms of Herpes

Step 1. Get to know the herpes virus further
The herpes virus has two strains, namely HSV-1 and HSV-2. Both are included in genital herpes. HSV-1 is the strain that mostly affects the lips and mouth, but it can also be spread through oral sex, just like HSV-2. There are several ways to relieve and overcome the symptoms of the disease caused by infection with the two strains of the herpes virus.
Treatment is an important part of disease control. If you don't treat genital herpes, you can pass it on to other people (including your unborn baby), develop bladder inflammation, rectal inflammation, and in severe cases, even meningitis

Step 2. Watch for symptoms about 2 weeks after being infected with herpes
Although you may have to wait a while for the initial symptoms to appear, the first attack is usually more severe than the subsequent herpes attacks. You may not even know you have herpes, so watch for any specific symptoms that start to appear. Flu symptoms are generally a sign of infection. These symptoms may include fever, muscle aches, decreased appetite, and fatigue. See your doctor if you suspect you are having your first herpes attack.
Because herpes symptoms take a long time to become apparent, some people may have a hard time realizing that their body has been infected with the disease. Or, because this disease can also be transmitted through people who do not show clear symptoms of herpes
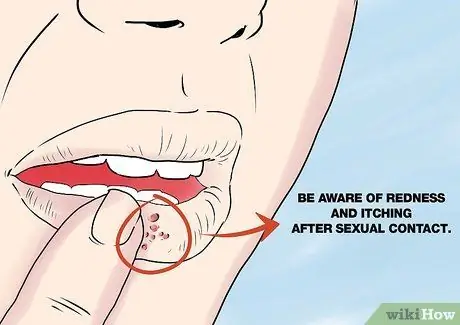
Step 3. Watch for redness and itching
After sexual intercourse, notice any redness or itching on your genitals or mouth. The skin affected by the virus may also feel a little stinging or hot. A few days later, your skin may appear rash. You should also be aware of external factors that may affect the onset of herpes after infection. These factors include:
- Trauma, stress, or menstruation. All of these conditions can cause the release of cortisol, adrenaline, and other stress hormones, or drastically alter hormone levels in the body. All of which can decrease the body's ability to fight infection, and give the virus a chance to cause disease.
- Burning and itching of the skin before herpes begins to attack (which is called prodromal). Relieves itching and burning when herpes is near to attack can speed up the attack. Scratching the itchy skin after a herpes attack occurs can increase the spread of the virus.
- Sunshine and fever. Ultraviolet exposure from sunlight can irritate the skin and disrupt core cells, thus providing an opportunity for herpes to attack. Fever or cold will weaken the body's immune system so that it is unable to fight infection, resulting in herpes attacks.
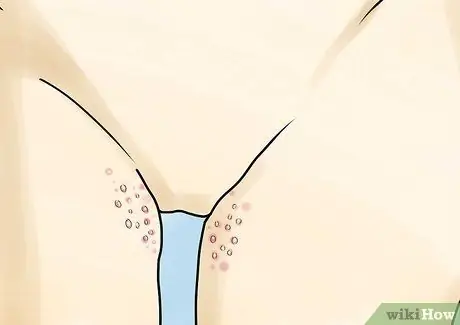
Step 4. Watch for prominent lesions on or around the genitals
You may notice raised lesions (bulles or vesicles) on the surface of the skin that appear about 6 to 48 hours after other herpes symptoms begin. If the lesion ruptures and becomes an open sore, you will see a cloudy fluid inside. Watch for prominent lesions on the lips, mouth, eyes, tongue, and other body parts. You may feel a stinging sensation before the prominent lesions begin to appear.
- In women, prominent lesions may be found on the labia, vagina, anus, cervix, buttocks, and thighs. Scabs will usually heal within 7 to 14 days.
- In men, prominent lesions are commonly found on the scrotum, penis, buttocks, and thighs.

Step 5. Watch for pain when urinating
During herpes attacks, you may feel pain when urinating. If you have difficulty urinating during your herpes outbreak--as some women have reported--seek medical attention. While this condition varies between female herpes sufferers, you should also pay attention to vaginal discharge (unusual or unnatural discharge).
Keep in mind that vaginal discharge is not a symptom that can diagnose herpes, but it is a possible symptom--along with other symptoms--can help make a diagnosis of herpes
Part 2 of 3: Seeking Medical Help and Controlling Herpes

Step 1. Visit a doctor or health clinic for an examination
If herpes strikes you at that time, your doctor may schedule an STD screening or take a sample culture to grow it. The doctor will then use the grown culture to check for herpes. Initial examinations that you should undergo include laboratory tests and scans.
- Usually, the diagnosis of herpes is made through a polymerase chain reaction (PCR) test of the test sample. The sample will be taken with a cotton swab that is rubbed vigorously on the affected skin. This sample will then be put into a liquid and sent to a laboratory. Then, using special laboratory techniques, the sample will be duplicated many times to check for the presence of herpes in the patient.
- In some cases, your doctor may order a herpes-specific antibody test. This test is performed using a specific antibody to target and determine whether the infection is caused by HSV-1 or HSV-2. Within 3 weeks of infection, 50% of patients are usually found to be positive for herpes. If you have been infected for more than 16 weeks, this test will also almost always give a positive result as well.
- The doctor may also consider a PCR test of a sample of a skin lesion. A sterile cotton swab will be used to gently wipe the base of the lesion-with pressure strong enough to remove epithelial cells without causing bleeding-and collect vesicular fluid. This sample is then sent to a laboratory for examination.

Step 2. Treat your symptoms with herpes antiviral medications
If the herpes test is positive, the doctor will prescribe medication to suppress the virus and relieve symptoms. Medication will also reduce the risk of transmitting the herpes simplex virus to other people. Start treatment for herpes immediately or do it as soon as possible, and use the drug as directed by your doctor. Herpes antiviral medications include:
- Acyclovir. Acyclovir is the drug of first choice for treating genital lesions or recurrent lesions on the labia caused by herpes. This drug can also be used topically to treat inflammation of the eye infected with herpes. Acyclovir is considered safe for use by pregnant and lactating women, as well as in children.
- Penciclovir. The drug in this cream preparation is used as the first choice to treat oral lesions topically.
- Valaciclovir. This drug is the first choice for treating primary and recurrent genital herpes.
- Foscarnet. This drug is considered a second choice and is used if herpes is resistant to acyclovir as the first choice. This can occur in cases of systemic herpes in patients with impaired immune systems.

Step 3. Cope with herpes attacks by taking control of your situation
Find out more about herpes, learn about this virus and how it is infected. The more you understand what's going on inside your body, the easier it will be to deal with and control its attacks. Herpes is a well-researched and well-documented disease. In fact, there is research still being done on herpes and the development of new drugs at this time.
Doctors also certainly have many sources of information about the latest herpes drugs for you

Step 4. Avoid transmitting the herpes infection
Take the time to explain your condition to your partner. Take precautions so as not to transmit the virus to others, which can generally be done by changing your lifestyle. For example, avoiding multiple sexual partners, using condoms between herpes attacks, and avoiding sexual intercourse during herpes relapses.
You should also not touch the herpes sores on the skin. If you touch it, wash your hands immediately with soap and water to kill the virus. Also, don't kiss anyone if you have an open sore in your mouth
Part 3 of 3: Considering High-Risk Behavior
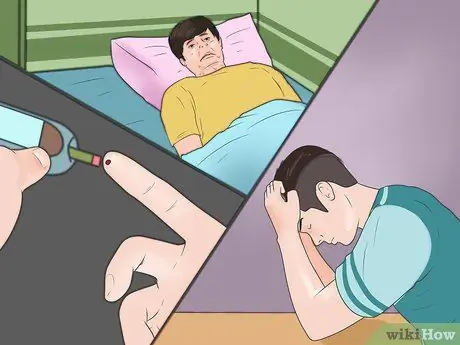
Step 1. Watch for high risk factors
Be aware that many people with genital herpes do not show symptoms for a long time. So, the high risk factors below can determine if you need a screening so you can get treatment early. Factors that increase your risk of getting herpes include:
- Decreased endurance. Although this condition itself doesn't cause herpes, it will make it harder for your body to protect itself and fight off infection or disease. Illness, stress, AIDS, cancer, diabetes, and even old age are factors that make your body more susceptible to infection with the herpes virus HSV-1/HSV-2.
- Atopic eczema in children (also known as atopic dermatitis). Eczema is itchy skin that is common, but if eczema on the skin is infected with herpes, serious skin diseases will occur.
- Exposure at work. Some workers who are exposed to the virus are at higher risk of developing herpes. For example, dentists are at a higher risk of becoming infected with HSV-1, which results in a particularly irritating infection of the hands.

Step 2. Recall whether you recently had unprotected sex
Sexual activity is a major risk factor for HSV-2. However, even safe sex can still transmit herpes, especially during relapses. Herpes spreads in the mucous layer (mucosa) of the skin, so the oral cavity, anus, penis, and vagina are at greatest risk of transmitting herpes. Herpes will be transmitted when one part of the body that is infected in a person comes into contact with the mucus layer of another person.
Touches that can easily transmit herpes include: oral, anal, and vaginal intercourse (or sexual intercourse where the mucus layers touch each other)
Step 3. Determine the number of your recent sexual partners
Because herpes can be transmitted through oral or genital contact, your chances of contracting the disease are proportional to the number of sexual partners you have had. The more sexual partners you have, the higher your risk of getting genital herpes.

Step 4. Understand the higher risk of infection in women
Women are more susceptible to herpes infection because it is more easily transmitted from man to woman than from woman to man. For example, the HSV-2 infection rate in women is 20.3%, while in men it is 10.6%.






