- Author Jason Gerald gerald@how-what-advice.com.
- Public 2024-01-19 22:11.
- Last modified 2025-06-01 06:05.
Neuropathy (dead nerves) of the feet indicates a disruption or malfunction of the small nerve fibers in both feet. Symptoms of neuropathy include pain (burning, electric shock and/or sharpness), tingling, numbness, and/or muscle weakness in the legs. Typically, peripheral neuropathy affects both legs, although sometimes not, depending on the cause. The main causes of foot neuropathy are uncontrolled diabetes, advanced alcoholism, infections, vitamin deficiencies, kidney disease, leg tremors, trauma, drug overdose, and exposure to certain toxins. Recognize the symptoms and signs of foot neuropathy to better understand the causes of problems in your feet. However, only a medical professional can give a definite diagnosis.
Step
Part 1 of 3: Recognizing Early Symptoms

Step 1. Take a closer look at your feet
You might assume that partial loss of sensation or sporadic tingling in the feet is normal and a part of aging, but it really isn't. Instead, it can be an early sign that the small sensory nerves in the feet are starting to malfunction. That's why check your feet more often and compare your feet' ability to feel light touch compared to other parts of your body, such as your thighs or hands.
- Use a pencil or pen to gently rub the feet (top and bottom) to assess sensitivity. Better yet, close your eyes and have a friend rub your feet.
- The loss of sensation/vibration usually starts in the toes and spreads slowly to the soles of the feet and eventually to the toes.
- In the United States, the most common cause of foot neuropathy is diabetes, with 60-70% of people with diabetes developing neuropathy in their lifetime.
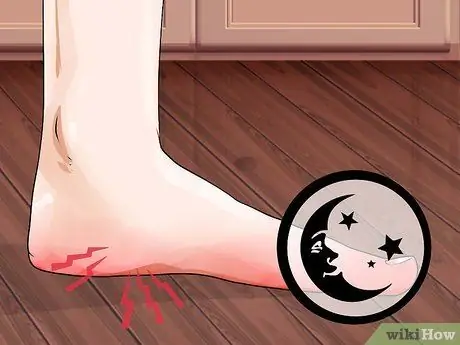
Step 2. Consider your leg pain
Some leg discomfort or cramping can be completely normal, especially after a long walk in new shoes, but constant burning pain or intermittent electric shock for no reason are early symptoms of foot neuropathy.
- Try to see if you notice any changes after changing your shoes, or try using ready made shoe inserts.
- Neuropathic pain usually gets worse at night.
- Sometimes, the pain receptors become so sensitive as a result of the neuropathy that even covering the feet is unbearable; This condition is called allodynia.
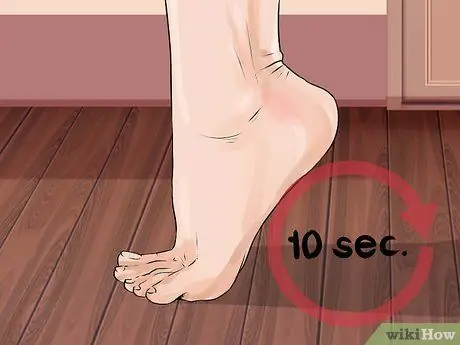
Step 3. Observe if the leg muscles feel weak
If walking becomes increasingly difficult or you feel more careless/stumbles more easily, this could be an early symptom of motor nerve damage in the foot due to neuropathy. Falling feet (inability to lift the front of the foot) while walking (which causes you to fall frequently) and loss of balance are also common symptoms of neuropathy.
- Try walking on your fingertips for 10 seconds and see how difficult it is for you. If it doesn't work at all, this could signal a problem.
- You may also notice the legs twitch on their own and lose their muscle tone.
- A brain stroke can also be caused by muscle weakness, paralysis, and loss of sensation in the legs, but these symptoms usually start suddenly and are accompanied by several other signs and symptoms, while neuropathy is usually gradual.
Part 2 of 3: Recognizing Advanced Symptoms

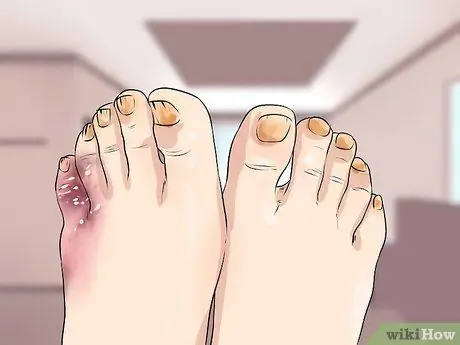
Step 1. Observe the discoloration of the skin and toenails
Further damage to the autonomic nerves in the feet tends to cause you to sweat less, resulting in less moisture in the skin (which causes dry, flaky, and/or chipped skin) and fingernails (making them more brittle). You may notice that your toes are starting to crumble and look like a fungal infection.
- If there are contaminants from arterial disease caused by diabetes, the skin on the lower legs may turn dark brown due to lack of blood flow.
- In addition to discoloration, skin texture can also change, often appearing smoother and shinier than before.
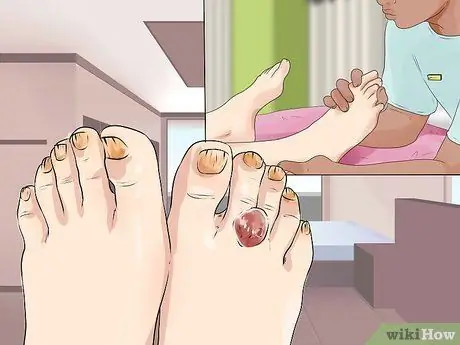
Step 2. Note the ulcer formation
Foot skin ulceration results from advanced sensory nerve damage. Initially, neuropathic ulcers are painful, but as sensory nerve damage progresses, their ability to transmit pain is greatly reduced. Repeated injuries can cause several ulcer formations that may go unnoticed by you.
- Neuropathic ulcers usually develop on the soles of the feet, especially for those who often walk barefoot.
- The presence of ulcers increases the risk of infection and gangrene (dead tissue).

Step 3. Watch for sensations that disappear completely
Legs that lose sensation completely are a big problem and should not be taken lightly. The inability to feel the sensation of touch, vibration, or pain makes it difficult for sufferers to walk and are vulnerable to the danger of foot trauma that can lead to infection. In the advanced stages of the disease, the leg muscles can become so paralyzed that it is completely impossible to walk unaided.
- Loss of sensation of pain and temperature can make the sufferer ignore when burned or accidentally cut. You may not realize that your leg is injured.
- Loss of coordination and balance makes you susceptible to leg, hip, and pelvic fractures from falls.
Part 3 of 3: Visiting a Medical Professional

Step 1. See a doctor
If you think your foot problem is more than just a minor sprain or sprain, and there are signs of neuropathy, you should see your doctor. He or she will perform a physical examination and ask about your history, diet and lifestyle. Doctors may also perform blood tests and check glucose levels (to look for signs of diabetes), certain vitamin levels, and thyroid function.
- You can also test your blood sugar at home with a commercial test kit, but make sure you read the user manual carefully.
- High levels of glucose in the blood is a poison that damages nerves and small blood vessels due to excessive consumption of ethanol from alcoholic beverages.
- Deficiency of B vitamins, especially B12 and folate, is another common cause of neuropathy.
- The doctor may also take a urine sample to assess the level of performance of the kidneys.

Step 2. Ask for a specialist referral
You may need the services of a neurologist (neurologist) to confirm the diagnosis of neuropathy. A neurologist may perform a nerve conduction study (NCS) and/or electromyography (EMG) to test the ability of the nerves in the feet to conduct electrical signals. Damage can occur in the protective covering of the nerve (myelin sheath) or under its axons.
- NCS and EMG do not help diagnose small neuropathic fibers so a skin biopsy or quantitative sudomotor axon reflex test (QSART) is sometimes used.
- A skin biopsy can reveal problems at the nerve fiber endings and is safer and easier than a nerve biopsy because the skin is on the surface.
- Doctors can also perform a color Doppler test to see the condition of the veins in the legs so that they can rule out venous insufficiency.
Step 3. Visit a podiatrist
A podiatrist is a foot specialist who can provide other information about foot problems. The podiatrist will check for trauma to the foot that could damage nerves or tame growths or tumors that irritate/compress nerves. A podiatrist can also prescribe custom shoes for you or orthotics for increased comfort and protection.
A neuroma is a benign growth of nerve tissue that is often found between the middle and ring toes
Tips
- Certain chemotherapy drugs are known to cause peripheral nerve damage, so ask your cancer doctor for side effects.
- Some heavy metals such as lead, mercury, gold, and arsenic can deposit on peripheral nerves and cause damage.
- Excessive and chronic alcohol consumption can lead to deficiencies in vitamins B1, B6, B9 and B12, which are important for nerve function.
- On the other hand, excessive consumption of vitamin B6 supplements can be harmful to the nerves.
- Lyme disease, shingles (varicella-zoster), herpes simplex, Epstein-Barr virus, cytomegalovirus, hepatitis C, leprosy, diphtheria, and HIV are types of infections that can cause peripheral neuropathy.






