- Author Jason Gerald gerald@how-what-advice.com.
- Public 2023-12-16 10:50.
- Last modified 2025-01-23 12:04.
Hives, or urticaria, are itchy rashes that appear on the skin. These nodules are often red and vary in size from about 0.6 cm to several cm in diameter. Most of these nodules will clear up with home treatments in about 1 day. However, if hives occur for more than a few days, you should see a doctor.
Step
Method 1 of 3: Eliminating the Trigger

Step 1. Remove the triggers of hives from your diet
You may need to record what foods you eat before and after changing your diet. These notes are needed to help you find the problematic food. There are several foods that can cause hives in some people:
- Foods containing vasoactive amines. This compound causes the body to release histamine, which triggers hives. Foods that contain this compound include shellfish, fish, tomatoes, pineapple, strawberries, and chocolate.
- Foods that contain salicylates. This compound is similar to aspirin, and foods that contain it include tomatoes, raspberries, orange juice, spices, and tea.
- Other allergens include peanuts, nuts, eggs, cheese, and milk. Hives can also be triggered by caffeine and alcohol in some people.
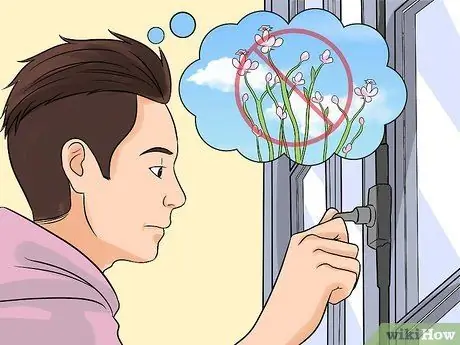
Step 2. Consider whether you are allergic to anything in the environment
If so, you may be able to treat hives by reducing contact with the material. Some people experience hives when exposed to the following ingredients:
- Pollen. If the trigger is pollen, you are more likely to develop hives when a lot of pollen is flying around. Try not to go out a lot during these times and close all windows in your home.
- Dust mites and animal dander. If you are allergic to dust mites, a completely clean, dust-free environment may help. Try vacuuming, dusting, and washing household appliances regularly. Change sheets to prevent you from sleeping on dusty sheets or animal hair.
- latex. Some people experience hives if exposed to latex. If you are a medical professional and suspect that your hives are latex, try wearing latex-free gloves to see if your hives can be treated.

Step 3. Avoid insect bites and stings
Some people experience hives due to insect compounds that enter the body through insect bites or stings. Some people even have severe allergic reactions and carry an epinephrine injection in case they get stung. When working outdoors, you can reduce your exposure to insect stings and bites by:
- Avoid beehives and wasps. If you see a wasp or bee approaching, don't try to fight it, but rather slowly move away and wait for it to fly away.
- Apply insect repellent to exposed clothing and skin. Do not allow these chemicals to enter your nose, eyes or mouth. There are many product options available, but products containing DEET are generally effective.

Step 4. Protect your skin from harsh environmental influences
You may need to protect yourself from extreme temperature changes until you can adjust to the new climatic conditions, or by wearing a stronger sunscreen. Some people with sensitive skin can experience hives due to several environmental factors, such as:
- Hot
- Cold
- Sunlight
- Water
- Pressure on the skin
Step 5. Discuss your treatment with your doctor
Some medications can cause hives in some people. If you suspect hives are triggered by a medication you are taking, do not stop using it immediately without consulting your doctor first. Your doctor may recommend other medications that can still treat your condition, but won't trigger hives. Medications that sometimes trigger hives include:
- Penicillin
- Some blood pressure medications
- Aspirin
- Naproxen (Aleve)
- Ibuprofen (Advil, Motrin IB, etc.)

Step 6. Consider your overall health condition
Talk to your doctor to determine if your hives are a symptom of another condition. A number of certain conditions can trigger hives in sufferers. These conditions include:
- Bacterial infection
- Intestinal parasites
- Viral infections, including hepatitis, cytomegalovirus, Epstein-Barr virus, and HIV
- Thyroid disorders
- Immune system disorders such as lupus
- Lymphoma
- Reaction to blood transfusion
- A rare genetic disorder that affects immune system function and blood proteins
Method 2 of 3: Using Natural Remedies

Step 1. Relieve skin irritation with a cold compress
A cold compress will relieve itching, so you don't need to scratch. You can compress with:
- Wet a washcloth with cold water and apply it to the surface of the skin. Leave it until the itching on the skin subsides.
- Glue the ice bag. If you use ice, wrap it first with a towel so it doesn't stick to the skin directly. Applying ice directly to your skin puts you at a higher risk of developing frostbite. If you don't have a bag of ice to work with, a bag of vegetables can be used instead. Apply the ice for about 10 minutes before removing it from your skin.

Step 2. Soak in cold water containing natural anti-itch remedies
This itching treatment has been around since time immemorial. Fill the tub with cold but comfortable water for you. Then, enter one of the following ingredients as recommended for use, and soak for a few minutes until your itching subsides.
- Baking soda
- Raw oatmeal
- Colloidal oatmeal (Aveno etc.)

Step 3. Wear soft, loose clothing to keep your skin cool and dry
Hives can be caused by skin irritation to clothing that is tight and keeps sweat from sticking to your skin. Loose clothing will help your skin breathe and prevent hives from developing from irritation and heat.
- Avoid wearing rough fabrics, especially wool. If you're wearing woolen clothing, try not to stick it directly to the skin. For example, by wearing a loose t-shirt on the inside when you wear a wool sweater.
- Similarly, sweat can irritate hives, bathing or hot baths too.

Step 4. Reduce stress
Some people experience hives when stressed. Consider whether there is a stressful event, such as losing your job, starting a new job, the death of a family member, moving, or problems in your relationship. If this is the case, learning to manage stress may help your hives. You can try:
- Meditate. Meditation is a relaxation technique that calms your mind. Take a few moments to close your eyes, relax, and release stress. Some people repeat a word in their mind while meditating.
- Take a deep breath. In this exercise, you should concentrate on inhaling until your lungs are completely full. Inhaling like this will relax you and prevent the shortness of breath that occurs when gasping for air. Deep breathing will also help you calm your mind.
- Visualize calming shadows. In this relaxation technique, you will imagine a calming place. The place can be real or just your imagination. When you imagine a place, you can walk around it and imagine its taste, smell and sound.
- Exercising. Exercising regularly can relax you, improve your mood, and improve your physical health. The US Department of Health and Human Services recommends that people get at least 75 minutes of physical activity a week. Strength training, such as lifting weights twice a week is also recommended.
Method 3 of 3: Seeking Medical Help

Step 1. Call the emergency room if you have trouble breathing
Sometimes people have difficulty breathing or feel their throat closing when they have hives. This condition is dangerous and you should call an ambulance immediately if you experience it.
If this happens, the ambulance staff will likely inject you with epinephrine. Epinephrine is a type of adrenaline and can deflate swelling quickly
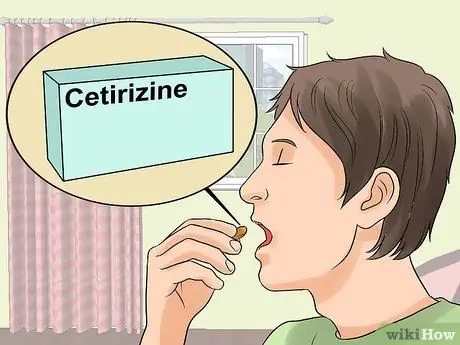
Step 2. Use an antihistamine
This drug can be purchased either with or without a prescription. Antihistamines are the first choice in treating hives, and are effective at relieving itching and swelling.
- Commonly used antihistamines include cetirizine, fexofenadine, and loratadine. Diphenhydramine (Benadryl) is a commonly used over-the-counter antihistamine.
- Antihistamines can make you feel drowsy, so talk to your doctor first to see if it's safe to drive while taking them. Do not drink alcohol while taking antihistamines. Read and follow the instructions on the packaging or the doctor's recommendations.
- Tell your doctor if you are pregnant. Antihistamines may not be safe for pregnant women.

Step 3. Ask your doctor about corticosteroids
This medication is usually prescribed if antihistamines don't work to relieve hives. Corticosteroids relieve hives by lowering your immune response. The most commonly prescribed corticosteroid is prednisolone for 3 to 5 days.
- If you have any of these conditions, tell your doctor before using corticosteroids to make sure they are right for you: high blood pressure, glaucoma, cataracts, or diabetes. Tell your doctor if you suspect you are pregnant or breastfeeding.
- Side effects include weight gain, mood disturbances, and insomnia.

Step 4. Try other remedies for hives that don't go away
If your hives do not subside after medical treatment, your doctor may refer you to a dermatologist. You may be given the option of trying other medications. Tell your doctor if you are pregnant or breastfeeding before using any medication.
- Menthol cream. You can apply this cream topically to relieve itching.
- H2 antihistamines. This medication is different from over-the-counter antihistamines and will constrict blood vessels, reducing swelling and redness. Side effects include headache, diarrhea, and dizziness.
- Leukotriene receptor antagonist. These drugs may be prescribed instead of corticosteroids because they tend to have less side effects. Possible side effects include headache and nausea.
- Cyclosporine. This medicine will suppress your immune system. Side effects include high blood pressure, headaches, kidney problems, high cholesterol, tremors, and making you more susceptible to attacks of infection. These drugs can usually only be used for a few months.
Step 5. Talk about light therapy with your doctor
Some cases of rash respond well to narrow-spectrum UVB light therapy. This treatment requires you to sit in a small room and be exposed to light for a few minutes.
- The effects of this treatment may not be felt immediately. You will have 2-5 treatment sessions per week, and it may take up to 20 treatment sessions before the effects are felt.
- This treatment can cause sunburn and increase the risk of skin cancer.
Warning
- If you are pregnant, nursing, or giving medication to children, consult your doctor before using any over-the-counter medications, herbal remedies, or supplements.
- Tell your doctor all medications, herbal remedies, and supplements you are taking. This is very important because these drugs can interact with other drugs.
- Read and follow the instructions on the medicine package, or all doctor's recommendations.






